Understanding Multiple Myeloma and Its Skin Symptoms
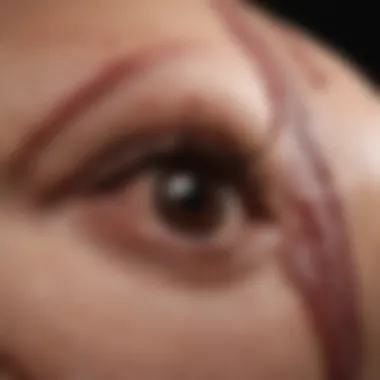

Research Overview
Key Findings
Recent studies shed light on the intricate relationship between multiple myeloma and skin manifestations. One particular study revealed that up to 30% of patients may show some form of skin-related symptoms, with variations ranging from benign to more severe conditions. The skin lesions often present as erythematous papules or nodules, which can significantly affect patients’ quality of life. Additionally, researchers have found that these lesions may not only signify disease progression but can also serve as indicators for treatment responsiveness.
Study Methodology
The findings primarily arose from a multi-center cohort study that enrolled 200 patients diagnosed with multiple myeloma over a span of five years. Researchers conducted detailed dermatological evaluations alongside standard oncological assessments. Clinical photographs were taken for documentation, and biopsies were performed on atypical lesions to investigate histological features associated with multiple myeloma. This comprehensive approach allowed researchers to correlate clinical findings with laboratory results, establishing a robust framework for future studies.
Background and Context
Historical Background
Multiple myeloma has been recognized as a distinct hematological malignancy since the early 20th century. Initially, the symptoms were largely attributed to bone marrow infiltration. However, as dermatological knowledge expanded, researchers started to observe skin lesions associated with the disease. The first notable publication highlighting these skin manifestations emerged in the 1950s, underscoring the need for a multidisciplinary approach in managing patients with multiple myeloma.
Current Trends in the Field
Today, the integration of dermatology into hematology is gaining traction. The emergence of targeted therapies is offering new hope, but they also bring forth unique side effects, including skin rashes and other dermatological symptoms. With the advent of immunomodulatory agents and proteasome inhibitors, practitioners are noticing a shift in the skin manifestations presented by patients. As treatment paradigms evolve, understanding these dermatological changes becomes paramount for optimizing patient care.
Prologue to Multiple Myeloma
Multiple myeloma, a complex hematological malignancy, has attracted significant attention due to its intricate nature and diverse manifestations. By understanding the fundamentals of this disease, especially its connection to skin and cutaneous symptoms, healthcare professionals can provide more comprehensive care. This section helps set the groundwork for the discussions that follow, illuminating why early recognition and appropriate intervention matter.
Understanding the Disease
To grasp multiple myeloma, one must first understand it as a malignancy of plasma cells, which are specialized white blood cells responsible for producing antibodies. When these cells begin to grow uncontrollably, they produce abnormal proteins that can lead to various health complications, including bone damage, kidney issues, and importantly, skin problems. Skin manifestations can sometimes be the window through which the broader disease is viewed, giving clues to the condition's severity and progression.
These phenomena illustrate the need for a thorough assessment of associated skin lesions. Recognizing how these lesions relate to multiple myeloma opens the door for better diagnostics and tailor-made treatment strategies that address not only the underlying disease but also the symptomatic experiences of patients.
Epidemiology and Demographics
Epidemiological studies show that multiple myeloma most commonly affects older adults, with a higher incidence in individuals aged 65 years and above. Interestingly, this disease appears to be more prevalent among African American populations compared to Caucasian individuals.
In the U.S., the lifetime risk of developing multiple myeloma stands at about 1 in 143, underscoring the importance of awareness and early detection. A few key points about its demographics include:
- Age: Risk increases significantly after age 60.
- Gender: Males are more frequently diagnosed than females.
- Ethnicity: African Americans experience the highest rates, while the condition is less common among Asian populations.
Understanding these demographic trends aids healthcare providers in identifying at-risk populations and formulating preventive strategies. Moreover, by exploring these statistical trends, we can foster discussions around health disparities and encourage a more nuanced understanding of multiple myeloma across various demographic groups.
Pathophysiology of Multiple Myeloma
The pathophysiology of multiple myeloma is crucial for grasping how the disease develops and the impacts it has on the body. This segment highlights the mechanisms and genetic factors contributing to the disease, which is essential for understanding both patient experiences and treatment options. In multiple myeloma, plasma cells, which are a type of white blood cell that produce antibodies, become malignant and start to proliferate uncontrollably. This overproduction disrupts normal immune function and leads to various clinical manifestations, including skin lesions.
Mechanisms of Plasma Cell Malignancy
Understanding the mechanisms that lead to plasma cell malignancy is foundational to grasping multiple myeloma. When plasma cells turn cancerous, they start multiplying without the checks and balances normally in place. This alteration typically starts with a disruption in the bone marrow environment, which becomes increasingly populated by these malignant cells.
A few critical elements contribute to this malignancy:
- Microenvironment changes: The bone marrow microenvironment plays a significant role in supporting tumor growth. Interactions with other cells, such as mesenchymal stem cells and immune cells, can encourage plasma cells to proliferate.
- Cytokine influence: Signaling molecules like cytokines and growth factors, such as interleukin-6, help these malignant cells survive and grow, further complicating the situation. High levels of these factors are often found in patients with multiple myeloma.
Furthermore, plasma cells often develop unique characteristics that allow them to evade the immune response. They produce a surplus of abnormal proteins, which can lead to kidney issues and other complications.
Genetic Mutations and Their Role
Genetic mutations are another cornerstone of the pathophysiology of multiple myeloma, providing insight into why certain individuals may develop the disease and others do not. Various genetic abnormalities have been identified in myeloma cells, and these can significantly affect how the disease responds to treatment.
Some key mutations include:
- Translocations: One of the most common genetic changes is the translocation involving the immunoglobulin heavy chain loci, specifically the t(4;14) translocation, which has been associated with a worse prognosis.
- Deletion of chromosome 17p: This deletion is linked to a more aggressive form of the disease and makes it harder to treat effectively.
These mutations promote malignant transformation and contribute to the disease's progression. Understanding these changes can open new avenues for targeted therapies designed to counteract these specific abnormalities.
Current research is focusing on identifying genetic profiles that may predict responses to therapies, highlighting the importance of personalized medicine in tackling multiple myeloma—this approach is progressively gaining traction.
In summary, the pathophysiology of multiple myeloma revolves around complex interactions between malignant plasma cells and their environment, coupled with significant genetic changes. Recognizing these elements provides the foundation for improved diagnostics and treatment strategies, offering insights that are vital for both clinicians and patients.

Skin Lesions in Multiple Myeloma
Understanding skin lesions occurring in patients with multiple myeloma is crucial for several reasons. Primarily, these lesions can serve as early indicators of disease progression and may also impact the overall well-being and quality of life of individuals affected by this condition. Recognizing these skin manifestations can assist healthcare professionals in prompt diagnosis and tailored treatment, ultimately improving patient outcomes.
Consequently, this section will delve into the various types of skin lesions associated with multiple myeloma and explore their implications on patient management.
Types of Skin Lesions
Cutaneous Plasmacytoma
Cutaneous plasmacytoma is a localized form of neoplastic proliferation of plasma cells that manifests primarily in the skin. These lesions are typically solitary and often appear as firm, well-defined nodules. One of the key characteristics that distinguish cutaneous plasmacytoma from other dermatological conditions is its tendency to occur in typically sun-protected areas of the body. This makes them significant for diagnostic considerations, as they can easily be mistaken for benign skin tumors or dermatofibromas.
The unique feature of cutaneous plasmacytoma lies in its clonal nature, usually being associated with the systemic disease of multiple myeloma, which highlights its relevance in the diagnosis. An advantage of identifying cutaneous plasmacytoma is that when properly diagnosed, it may respond favorably to local therapies, such as radiation treatment. However, its disadvantage includes the need for comprehensive patient evaluation to rule out concurrent systemic disease, as mismanagement can lead to poor clinical outcomes.
Non-specific Dermatitis
Non-specific dermatitis in multiple myeloma encompasses a range of inflammatory skin conditions that do not have a precise etiology but commonly appear in patients diagnosed with the disease. This type of dermatitis often presents as eczematous patches and has a multifactorial nature that may involve drug reactions, systemic disease, or even secondary infections.
A key characteristic of non-specific dermatitis is its variable presentation, which can lead to confusion regarding its underlying cause. It is beneficial to recognize these lesions as they often respond to symptomatic treatment but can also signify disease exacerbation or complications from treatments. A noteworthy advantage is the potential for improvement with topical corticosteroids; however, a disadvantage includes that it can decrease the patient’s quality of life due to discomfort and psychological stress related to visible skin changes.
Thrombocytopenic Purpura
Thrombocytopenic purpura, commonly linked with low platelet counts, manifests as easy bruising or bleeding beneath the skin surface. This condition arises from both the myeloma itself, which can interfere with platelet production, and the treatments associated with managing multiple myeloma. Its crucial aspect is that these lesions can be indicative of serious underlying complications related to the disease.
A key characteristic of thrombocytopenic purpura is its presentation as petechiae or larger ecchymosis. This condition becomes particularly significant as it not only serves as a marker for hematologic instability but also poses a risk for serious bleeding episodes, thereby influencing treatment decisions. The advantage of recognizing this manifestation early allows for timely interventions, such as platelet transfusions or modifications in therapy. However, one must be cautious as it complicates anti-cancer treatments, leading to potentially severe outcomes.
Pathology of Skin Manifestations
The pathology associated with skin manifestations in multiple myeloma is intricate and a focal point of ongoing research. Various skin lesions differ significantly in their histopathological findings, contributing valuable insights into patient management. These findings often provide a clearer understanding of how the disease evolves and reacts to treatments, fostering improved therapeutic strategies. Moreover, exploring these mechanisms underscores the pressing need for heightened awareness of the skin changes accompanying multiple myeloma, ultimately driving enhanced clinical practice and patient education.
Symptoms and Patient Experiences
Understanding the symptoms and patient experiences in the context of multiple myeloma is crucial for several reasons. Not only do these manifestations highlight the complexities of the disease itself, but they also inform treatment options and patient management strategies. Recognizing the physical and emotional toll that multiple myeloma can impose sets the groundwork for developing comprehensive care plans tailored to individual patient needs.
The interplay between the physical symptoms and the psychosocial impact on patients forms a significant part of their journey through diagnosis and treatment. Each experience is unique, shaped by various factors including age, comorbidities, and personal support networks. This section digs into two fundamental aspects: the physical symptoms and the psychosocial impact, both of which play pivotal roles in defining a patient's quality of life.
Physical Symptoms
Patients with multiple myeloma often exhibit a wide range of physical symptoms, many of which stem from the disease's influence on the bone marrow and skeletal system.
Common physical manifestations include:
- Bone pain: This is one of the most frequently reported symptoms. The pain is typically localized to the back or ribs and may result in significant discomfort.
- Fatigue: Patients frequently complain of exhaustion. This isn’t just ordinary tiredness; it can be a profound lack of energy that hampers daily activities.
- Anemia: The reduction in red blood cells can lead to paleness, weakness, and increased heart rates. Some individuals might feel dizzy or breathless even with minimal exertion.
- Renal impairment: Kidney function can decline, leading to additional symptoms like swelling in the legs or elevated blood pressure.
- Increased susceptibility to infections: As multiple myeloma affects the immune system, patients might find themselves getting sick more often.
These symptoms can interact in complex ways, often exacerbating one another. For instance, the fatigue caused by anemia may limit a person's ability to manage pain effectively, which can lead to further isolation and despair. Recognizing the interconnectedness of these physical symptoms is vital for healthcare providers aiming to offer effective interventions.
Psychosocial Impact
The psychosocial repercussions of a multiple myeloma diagnosis cannot be overlooked. The emotional and mental health aspects deserve as much attention as the physical symptoms.
Living with a chronic illness can lead to a myriad of psychological challenges, including:
- Anxiety and depression: Patients may feel constant worry about their health, treatment processes, and future. This can manifest as chronic anxiety, leading to depressive states.
- Social withdrawal: Fearing the stigma associated with visible symptoms can make patients retreat from social circles, leading to feelings of isolation. This is especially true for those experiencing skin manifestations.
- Impact on self-esteem: Physical changes, whether through body image shifts from weight loss or symptoms affecting skin appearance, can dent self-confidence, leading to further psychological distress.
- Family dynamics and burden: Patients often struggle with their roles in family life. The burden of their illness can put a strain on relationships, causing tension in what was once a supportive environment.
The combination of physical suffering and psychosocial distress can create a vicious cycle, each exacerbating the other. Addressing both aspects simultaneously is critical for improving a patient’s overall wellness.
Research indicates that holistic management approaches benefit multiple myeloma patients. This means integrating mental health support, pain management, and social engagement strategies into the treatment plan. Engaging with supportive community resources, including counseling and support groups, can significantly improve patient experiences and outcomes.
In sum, the symptoms tied to multiple myeloma go far beyond the physical realm. By embracing a comprehensive view of both the physical symptoms and the psychosocial dimensions, stakeholders involved in patient care can enhance the quality of life for those battling this complex disease.
Diagnosis of Skin Lesions
In the journey through multiple myeloma, diagnosing skin lesions stands as a crucial milestone. Among various symptoms displayed by patients, skin manifestations can often serve as the very first indicators of underlying complications, thus rendering accurate diagnosis essential. A well-structured diagnostic protocol not only expedites treatment but also plays a significant role in monitoring disease progression.
Skin lesions, be they cutaneous plasmacytomas, dermatitis, or purpura, necessitate a meticulous evaluation. Prompt and thorough diagnosis can lead to timely interventions, which are invaluable in improving the overall quality of life for patients.
Clinical Evaluation


The cornerstone of diagnosing skin lesions in multiple myeloma lies in clinical evaluation. Healthcare providers need to embark on a comprehensive assessment that combines patient history, symptomatology, and physical examination. Clinicians should look for specific characteristics of skin lesions – their appearance, distribution, and duration. Often, the skin may give away more than what meets the naked eye, revealing the systemic nature of multiple myeloma.
During clinical evaluation, practitioners might consider the following:
- Patient history: Previous skin conditions, family history of skin diseases, and any recent medical treatments.
- Skin examination: A detailed look is needed, noting the number, size, color, and texture of lesions.
- Symptom inquiry: Patients should be asked about itchiness, pain, or other discomforts related to the skin lesions, all of which can guide to a more profound understanding.
Histopathological Examination
If the clinical evaluation raises suspicion, a histopathological examination becomes essential in confirming the presence of malignancies such as cutaneous plasmacytoma. Skin biopsies provide a window into the cellular architecture of the lesions, allowing for detailed microscopic analysis. This examination not only aids in determining the nature of the skin lesion but also helps differentiate it from other dermatological disorders.
Histological features that may be examined include:
- Presence of plasma cells within the tissue samples, typically indicative of cutaneous plasmacytoma.
- Morphological changes in skin compartments, revealing any abnormal growth or infiltration.
- Inflammatory responses that could elucidate underlying medical conditions.
Ultimately, histopathological results give clinicians valuable data, directing appropriate treatment plans.
Differential Diagnosis
Establishing a differential diagnosis for skin lesions associated with multiple myeloma requires a systemic approach. Given the overlapping symptoms with various skin diseases, differentiating between them becomes vital. By recognizing these, one can avoid misdiagnosis, which can delay commencement of crucial therapies.
Common conditions that need consideration during differential diagnosis include:
- Drug eruptions: Skin reactions from chemotherapeutic agents may mimic myeloma lesions.
- Infections: Bacterial, fungal, or viral infections can present skin symptoms similar to those caused by multiple myeloma.
- Other malignancies: Skin cancers such as melanoma or squamous cell carcinoma need to be ruled out.
In this regard, effective diagnosis hinges on a thorough clinical assessment and collaboration with dermatologists to ensure the accurate identification of the underlying issues. Engaging in a dialogue about the diagnostic methods can facilitate better patient outcomes and shed light on the complexities of multiple myeloma.
Treatment Approaches
Treatment Approaches play a crucial role in managing multiple myeloma and its associated skin manifestations. Proper interventions can not only help control the underlying hematologic condition but also alleviate the discomfort and distress caused by skin lesions. Hence, understanding various methods available for treatment is essential for clinicians and patients alike. In this section, we'll discuss pharmacological treatments and emerging therapies, detailing their significance and how each contributes to patient care.
Pharmacological Treatments
Pharmacological treatments form the backbone of therapy in multiple myeloma. They vary widely in their mechanisms and effectiveness, each with its own set of attributes that render it beneficial in specific patient situations.
Corticosteroids
Corticosteroids, like dexamethasone and prednisone, are commonly used in the management of multiple myeloma. They work by suppressing immune function and reducing inflammation, making them effective in treating skin manifestations as well. One key characteristic of corticosteroids is their rapid onset of action—often providing significant relief within days. This swift response is particularly valuable for patients experiencing discomfort from skin lesions.
Corticosteroids are popular choices due to their effectiveness and availability in various formulations, from topical applications to systemic administration. However, it's important to consider potential downsides. Long-term use can lead to side effects like osteoporosis, weight gain, and increased susceptibility to infections. This necessitates careful monitoring and weighing of risks versus benefits in each patient.
Targeted Therapy
Targeted therapy is a more recent addition to the arsenal against multiple myeloma. This approach specifically targets the molecular mechanisms driving the disease, sparing normal cells and reducing side effects associated with traditional chemotherapy. For instance, agents like bortezomib and carfilzomib inhibit proteasome activity, which is crucial for cancer cell survival.
The key characteristic of targeted therapy is its precision. By homing in on specific pathways involved in multiple myeloma, it potentially offers better outcomes with fewer adverse effects. The uniqueness of these therapies lies in their ability to target cancer growth in a more personalized manner; however, their effectiveness can be influenced by genetic factors within individual tumors. Therefore, while targeted therapy is beneficial, it also requires genetic profiling that can be a barrier for some patients.
Chemotherapy Regimens
Chemotherapy has been a mainstay in treating multiple myeloma for decades. Regimens often combine several drugs to maximize efficacy. Commonly used agents include melphalan and cyclophosphamide, which work by damaging DNA in rapidly dividing cancer cells. The hallmark of chemotherapy is its ability to achieve deep responses, yet it can come with considerable downsides.
One major feature of chemotherapy is that it can be administered in different cycles. This cyclic approach allows doctors to monitor effects on skin lesions and adjust treatments as needed. However, side effects like nausea, hair loss, and increased infection risk make it essential to monitor patients closely. The advantage of chemotherapy lies in its proven track record in managing multiple myeloma, but the downside often requires supportive therapies and close patient management.
Emerging Therapies
As research into multiple myeloma advances, so too do the treatment options available to patients. Emerging therapies represent the forefront of science, exploring innovative ways to tackle this complex disease. These therapies often include monoclonal antibodies, CAR T-cell therapy, and immune checkpoint inhibitors, shifting treatment paradigms towards more personalized options.
One noteworthy aspect of these therapies is their potential to offer novel treatment paths for patients who have exhausted traditional options. The unique characteristic of emerging therapies is their mechanisms, which focus on harnessing and enhancing the body’s immune response against myeloma cells, therefore potentially leading to durable remissions.
However, the integration of these new therapies can come with challenges, including cost and access limitations. Furthermore, long-term data on their safety and efficacy are still being gathered, which makes the conversation around using emerging therapies rich with both hope and caution.
In summary, the treatment landscape for multiple myeloma and its skin effects is as complex as the disease itself. Understanding the varied approaches not only aids healthcare professionals in making informed decisions but also empowers patients to engage actively in their treatment journey.
Management of Skin Lesions
Managing skin lesions in patients with multiple myeloma is a nuanced endeavor that warrants careful consideration. The skin manifestations can often serve as a visible marker of systemic disease progression, creating a complex interplay between treatment needs and patient quality of life. Effectively addressing these lesions not only alleviates discomfort but also plays a significant role in overall patient management. Without a proper focus on these aspects, the cumulative adversity faced by patients could adversely affect their emotional and physical well-being.
Topical Interventions


Topical interventions encompass a variety of approaches aimed at managing skin lesions resulting from multiple myeloma. These treatments can include ointments, creams, and lotions that aim to relieve symptoms while exerting therapeutic effects on the lesions themselves.
- Corticosteroids serve as frontline treatments for inflammatory skin lesions. They can significantly reduce redness, swelling, and itching, providing quick relief for patients.
- Moisturizers play a vital role in hydrating dry or compromised skin. Their use can prevent further irritation and help bolster the skin barrier.
- Antihistamines can be added to the mix to tackle any itching or discomfort, ensuring that patients maintain a semblance of quality in their day-to-day life.
While these interventions can yield positive results, patient adherence is crucial. It’s paramount for healthcare providers to educate their patients about the importance of consistent application and follow-through. Moreover, understanding that some topical agents may cause skin irritation is essential in tailoring an appropriate management plan.
"The skin can often reflect a patient’s internal disease state, ensuring attention to these lesions is critical for treatment efficacy and emotional resilience."
Surgical Options
In scenarios where topical treatments do not yield satisfactory results, or when lesions pose risks of complications or malignancy, surgical options may become necessary. Surgical interventions can range from minor procedures to more invasive operations depending on the nature of the skin manifestation.
- Excision of Lesions is a routine surgical approach for cutaneous plasmacytomas. A skilled surgeon removes the lesion while ensuring clear margins to reduce recurrence rates. Proper follow-up care is needed to monitor for any signs of regrowth.
- Cryotherapy which involves freezing the lesions, can serve as an alternative management strategy. This technique is noteworthy for its minimal invasiveness and potential effectiveness for select lesions.
Surgical options can have a significant impact on a patient’s psychological state as well, from enhancing self-esteem to improving overall quality of life. However, they also require a well-structured follow-up plan, as the risk of complications can arise.
Prognosis and Quality of Life
Understanding the interplay between prognosis and quality of life is vital in grasping the full scope of multiple myeloma's impact on patients. Prognosis refers to the expected course and outcome of the disease, while quality of life encompasses the overall well-being, covering physical, emotional, and social aspects. The relationship between these two elements reflects how patients navigate through their diagnosis and treatment journey.
The prognosis for multiple myeloma can vary significantly from patient to patient, influenced by factors such as age, overall health, genetic mutations, and response to initial therapy. Generally, advancements in treatments have improved survival rates, leading to a more hopeful perspective for many. Nevertheless, each individual's experience is unique, and interpreting survival rates without considering quality of life can be misleading.
Benefits to understanding prognosis include:
- Tailored Treatment Plans: Knowing one's prognosis can aid in crafting personalized treatment strategies aimed at maximizing survival while considering the side effects that may interfere with daily functioning.
- Preparedness: Outlining prognosis can equip patients and their families to manage expectations, make informed decisions, and engage in advance care planning.
- Emotional Resilience: Gaining clarity about the future allows patients to focus efforts on quality of life improvements rather than merely surviving.
Considerations for quality of life are equally essential. When managing multiple myeloma, patients may experience physical discomfort from symptoms or treatment side effects, which directly affects their emotional well-being and social interactions. Recognizing how prognosis impacts quality of life allows healthcare providers to address both dimensions effectively.
"Quality of life in multiple myeloma patients is not just about the years added to life; it's also about the life added to years."
Patients often face challenges such as pain, fatigue, anxiety, and social isolation stemming from their condition. These factors can severely limit their daily activities, resulting in feelings of inadequacy and helplessness.
Improving quality of life can involve holistic strategies, such as:
- Pain Management: Properly addressing pain to maintain daily activities.
- Psychosocial Support: Psychological counselling and peer support groups can help bridge emotional gaps.
- Nutritional Interventions: A well-balanced diet can support physical health and energy levels.
Thus, evaluating both prognosis and quality of life provides a complete picture, enabling healthcare professionals to offer comprehensive care that acknowledges the intricate realities faced by multiple myeloma patients.
Future Directions in Research
Innovations in Treatment
Continuing advancements in medical science have paved the way for innovative treatment methodologies for multiple myeloma. Here are a few key areas to focus on:
- Monoclonal Antibodies: These have become essential in treating various blood cancers. New developments are in full swing to enhance their efficacy in targeting malignant plasma cells while minimizing side effects.
- CAR T-Cell Therapy: Engineered T-cells expressing chimeric antigen receptors show promise in eliminating myeloma cells. This therapy’s potential to provide long-lasting responses is being closely monitored.
- New Drug Trials: Ongoing clinical trials are assessing drugs that target specific pathways of myeloma cell growth and survival. Understanding these pathways better may cultivate improved treatment combinations that can tackle the disease aggressively.
Looking forward, these innovations could transform patient management and tailor treatments that cater to individual genetic profiles.
Understanding Disease Progression
Grasping the nuances of how multiple myeloma progresses is equally important. Recent studies emphasize the need to delineate the phases of this disease better. Research increasingly focuses on:
- Biomarkers for Early Detection: Identifying reliable biomarkers can lead to early diagnosis, ultimately improving prognosis. Understanding how certain markers correlate with disease progression can also offer insights into a patient’s specific disease trajectory.
- Microenvironment Factors: The interaction between plasma cells and their surrounding microenvironment may play a crucial role in disease advancement. Investigating these dynamics can aid in creating microenvironment-targeted therapies.
- Longitudinal Studies: Collecting data over time from diverse patient populations can illuminate patterns in disease progression. This observational approach helps in developing a nuanced comprehension of disease behavior, which in turn guides clinical decisions.
In summary, tapping into these future directions in research holds great promise for enhancing treatment strategies and optimizing care for patients with multiple myeloma. As the landscape of medical research continues to shift, both clinicians and patients will benefit from an approach that emphasizes innovation and a deeper understanding of this complex disease.
Ending
Multiple myeloma, primarily a hematological malignancy, often presents with symptoms that extend beyond the blood and bone marrow environments. The skin manifestations can serve as barometers of the disease's progression and can affect the overall quality of life. Recognizing these lesions and comprehending their implications can lead to timely interventions and tailored treatments, ultimately influencing patient outcomes.
By synthesizing the information presented, we highlight the necessity of ongoing education and vigilance within the healthcare community. The intersection of dermatology and hematology in multiple myeloma warrants further consideration and emphasizes the multidisciplinary nature of caring for patients.
Key Takeaways
- Multiple myeloma can present with various skin manifestations, which are not mere cosmetic issues but significant indicators of the disease’s severity and progression.
- Skin lesions, such as cutaneous plasmacytomas or non-specific dermatitis, necessitate a thorough understanding for effective diagnosis and treatment.
- Timely diagnosis and effective management of skin symptoms can enhance the quality of life for affected patients.
- The collaboration between specialists in both dermatology and oncology becomes essential when treating patients.
Call for Further Research
There exists a notable gap in the literature regarding the comprehensive management of skin manifestations in multiple myeloma. Future research should focus on:
- The mechanisms by which multiple myeloma affects skin health and the biology behind various skin lesions.
- The efficacy of emerging treatment modalities specifically targeting the skin aspects of the disease.
- Longitudinal studies to track the impact of skin lesions on patient quality of life and overall survival.
- Development of interdisciplinary approaches that integrate dermatological evaluation in routine multiple myeloma management.
Addressing these areas through structured research will not only improve patient outcomes but also enrich the understanding of multiple myeloma as a multifaceted disease.







